Breast Cancer in White American Women Peer Reviewed
Review Article Clinical Review
Breast Cancer Screening in Older Women: The Importance of Shared Decision Making
The Journal of the American Board of Family Medicine May 2020, 33 (3) 473-480; DOI: https://doi.org/ten.3122/jabfm.2020.03.190380

Abstract
Incidence of breast cancer increases with historic period up until age fourscore. Screening mammography has demonstrated efficacy in decreasing bloodshed from breast cancer among women between 50 and 74 years of age. However, most major organizations practise not include women over 74 in their recommendations due to the lack of evidence in this age-grouping. This article will review electric current recommendations for breast cancer screening in women over the age of 74. It volition also present clear guidelines for primary care clinicians to follow that incorporate shared controlling techniques, tools for estimating the risks and benefits of screening mammography, and strategies for integrating a patient'south life expectancy and comorbidities into the decision-making procedure. We also emphasize the importance of using thoughtful communication strategies to fully engage older women in the breast cancer screening discussion.
- Breast Cancer
- Communication
- Early on Detection of Cancer
- Incidence
- Mammography
- Primary Health Intendance
- Risk Assessment
- Shared Decision Making
Instance
Ms. Brownish is a 76-year-erstwhile woman with well-controlled hypertension merely no other medical problems. She comes in for a physical. You bring up breast cancer screening and discuss the mixed recommendations for standing screening mammography in women over 74. What should you tell her?
Groundwork
Historic period is the major chance cistron for chest cancer. Breast cancer accounts for thirty% of all new cancer diagnoses in women.1 Breast cancer deaths have declined significantly in the U.s. due to improvements in early detection and treatment efficacy, but breast cancer still accounts for 30% of all new cancer diagnoses in women.1 Approximately 41% of all incident chest cancers and 57% of all breast cancer deaths occur among women aged 65 years and older.ii Furthermore, women ≥ 65 who develop breast cancers accept college death rates and poorer outcomes.3⇓–v The incidence of breast cancer continues to increment until age lxxx.vi
Screening mammography has been shown to exist effective in reducing breast cancer mortality in women aged l to 74 years.three However, because none of the randomized trials of screening mammography included women over the historic period of 74, and very few trials included women over the age of 70, screening recommendations for older women are defective and remain controversial. The decision to keep screening in women over the age of 74 should be individualized, taking into account potential benefits and harms of screening in the context of a woman's overall health, life expectancy, and values. This article aims to provide a guide for main care clinicians who take care of women over the age of 74.
Screening Guidelines for Women over 74
Most guidelines suggest that chest cancer screening should continue until the age of 74, but beyond that age, professional organizations differ in their recommendations (Table 1). The American Cancer Lodge advises physicians to go along screening patients as long as they are in "proficient overall health" and have a life expectancy of 10 year or longer,vii whereas the American College of Physicians recommends screening finish at historic period 74.viii The United states of america Preventive Services Task Force offers no recommendation, due to insufficient show.9
Table 1.
Summary of Screening Mammography Recommendations in Older Women at Average Risk
Benefits and Harms
Although randomized trials did not include women over the age of 74, observational studies have shown a reduction in breast cancer mortality associated with mammographic detection of breast cancer in women 75 years and older.10 Modeling studies have also shown that continuing biennial screening to age 79 years (vs 69 years) reduces breast cancer bloodshed by six% to ten%.11 When biennial screening mammography is connected into a woman's 70s (rather than until age 69), 2 fewer women per one thousand die from chest cancer subsequently x years.12 The specificity and sensitivity of mammography improves with older age. Mammography in women older than lxxx years has a sensitivity of 86% and specificity of 94% (vs sensitivity = 73% and specificity = 92% in 50-yr-onetime women).13 As women historic period, the proportion of invasive ductal cancer versus ductal carcinoma in situ cases rises, while the proportion of cases with positive nodes decreases.14 Elderly women who forgo screening are more likely to present with highest stage cancersfour,xv,xvi and show reduced survival.iv,18⇓–twenty Therefore, the nigh obvious benefit of standing screening in older women is finding breast cancer at a signal when potentially harmful handling can be minimized, life expectancy maintained, and morbidity avoided.
The potential harms of chest cancer screening in older women include imitation positive results and overdiagnosis. Among women 75 years and older, 200 out of 1000 who are screened over ten years will experience a false alarm,10 which tin cause pain, feet, and distress.21,22 False positive mammogram results decrease with age.12 Overdiagnosis, a phenomenon in which a cancer detected by screening would not have gone on to cause symptoms or expiry, is a harm of screening that increases with age.ten,23,24
Follow-up procedures such as additional mammograms, ultrasounds, and breast biopsies may be more painful and frightening for older women who accept cognitive harm (dementia) and other comorbidities (arthritis, hemiparesis).22,25,26 Farther, treatments for breast cancer (surgery, chemotherapy, and radiation) may confer greater risks in older women and impact their quality of life without prolonging their life.
Information technology is important to communicate the possible harms of breast cancer screening to patients, because many older adults tend to overestimate the benefits of screening and underestimate the harms.27,28
Taking into Account General Health, Comorbidity, and Life Expectancy
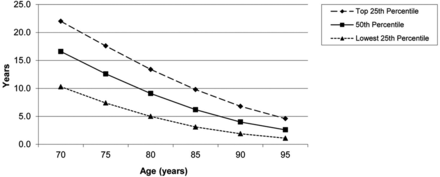
Several guidelines recommend screening women who have a life expectancy of at least 10 years and skilful overall health (Table i). Based on 2008 US Life Tables, approximately l% of 80-year-old women and 25% of 85-year-one-time women will live at to the lowest degree x years (Figure 1).ten,29
Studies show that chest cancer screening does not benefit older women with severe or multiple comorbidities, due to competing causes of mortality.4,16,20 Although women with a life expectancy of less than 10 years are unlikely to experience a bloodshed reduction from screening mammography,7,9,10,30 many women with serious comorbidities are still receiving routine screening mammograms.31,32 Amid older women, chest cancer chance factors such as lifelong obesity, loftier os density, and high breast density are also more predictive of late-life breast cancer than factors such as age at first nascence or age at first menarche.10
An algorithm included in this article can assist guide the conclusion-making process (Figure 2). Another resource that may exist helpful for physicians is ePrognosis (https://eprognosis.ucsf.edu), a repository of geriatric prognostic indices. These indices incorporate age, comorbidities, and functional condition to predict long-term mortality among older women and can be used to approve clinical judgment.33 For instance, a adventure estimator on the ePrognosis website tin be used to guess a woman's probability of living for 10 years or longer by inputting information about the patient'south age, BMI, past medical history, and ability to perform normal daily activities. If the 10-twelvemonth mortality risk is calculated as <50%, the life expectancy is estimated to be greater than 10 years, and screening may exist recommended to the patient. Another pick on ePrognosis is an online breast cancer screening aid. This tool requires input of like patient information as the risk calculator and so offers a screening recommendation on the final folio. Information that a patient may find useful, such equally supporting data virtually benefits and harms of screening, the run a risk of false positives, and mortality estimates, accompanies the recommendation.
- Download figure
- Open in new tab
Figure 2.
Life expectancy of women in the United States.10 This figure shows that historic period alone is a crude predictor of life expectancy because considerable variability in longevity exists among women in the The states.
Strategies for an Effective Word
Because the decision to continue breast cancer screening in older women should be about appropriately individualized, it is important to use a shared controlling process with the patient. Data show that patients appreciate discussions of stopping screening most from a trusted clinician. Therefore, these conversations should accept place betwixt the principal care physician and the patient. It is logical to start discussing when to cease screening as a woman nears 74, which is when the recommendations modify. That style, the clinician and patient can take a series of conversations about the topic of screening, how often to screen, and when or whether to end screening at a certain age. Screening conversations can besides include a partner or family unit member who can help delineate wellness priorities.
Cardinal shared decision-making elements for the clinician are discussing both the risks and benefits of mammography and so assessing the patient's understanding of the information presented.34 Conveying numbers using absolute risk reduction, natural frequencies, and descriptive, everyday language (rather than technical jargon) will as well better the patient's comprehension.35 When discussing breast cancer screening, it is necessary to explore the patient's preferences as well. For instance, screening mammography should not exist performed on women who would not choose further evaluation or treatment based on aberrant screening results. In addition, some patients may find niggling value in the slight mortality benefit that screening offers and may wish to avert the potential harms of screening.
Health decision aids are a helpful tool for presenting data about screening mammography to women. They frequently include visual aids and present risk with accented risk reductions instead of relative risk reductions, to maximize the patient's agreement. Beth State of israel Deaconess Medical Centre offers 2 decision aids for older women, 1 xfor women anile 75 to 84 and another for women anile 85 or older.36⇓–38 The Center for Medical Psychology and Evidence-Based Decision-Making also offers a decision assist for women lxx years or older.39 These decision aids can exist printed out, and they offer more detailed information than the online ePrognosis breast cancer screening aid. The University of Sydney tool is a 24-page interactive worksheet geared specifically for women over 70 that women tin print out and work through (http://www.psych.usyd.edu.au/cemped/docs/Mammogram_DecisionAid.pdf).39
Case (Continued)
Nosotros go through the decision help with Ms. Dark-brown. She has well-controlled hypertension, does not smoke, and can walk iii blocks with no assistance. She has not been admitted to the hospital in the last yr. The decision assist assigns points to each question (ie, have yous ever been diagnosed with cancer, tin you walk 3 blocks), and the lower the score (the more negative answers), the more likely that the potential benefits of a mammogram will outweigh the potential harms. Based on her overall good wellness, it is likely that she would continue to benefit from screening if she decides to continue.
Boosted aids tin be constitute on the Ottawa Patient Conclusion Aids Inventory.40 A case study is included in this article that shows how to use the Beth State of israel health decision aid for women anile 75 to 84,37 and elements of the iii-talk shared conclusion-making model,41,42 to hash out chest cancer screening with older women (Box 1). The iii-talk model is a method of ensuring that shared conclusion making is taking identify. It makes sure that the clinician includes a statement about the choice that needs to be made (choice talk), the options to choose between (option talk), and so concludes with a conclusion that is adherent to the patient's values (decision talk).
BOX i:
Example—using a health decision assistance and the 3-talk model to discuss breast cancer screening in older women
Jane Brownish is a 76-year-old woman presenting for a concrete. She has well-controlled hypertension, lives on her own, and maintains a physically active lifestyle. Jane has been getting biannual screening mammograms for many years and finds them reassuring because she has personally known women with chest cancer. At this appointment, Jane is wondering if she needs to schedule a screening mammogram.
1. Choice Talk
You let your patient know that she can continue with biannual screening, or stop screening altogether, and that you tin work with her to attain a decision that would be best for her. To start, you tell her that it is unclear if screening mammograms benefit women over the historic period of 74, and you explain why. Then, you offer to talk over her overall health, life expectancy, and personal preferences together with her to decide whether to keep, or stop, biannual screening.
Example: Beyond age 74, it is unknown whether women benefit from routine screening mammograms. This controversy exists because trials of screening mammography did non include women over the age of 74. Some organizations say that women should cease screening when they are 74 years old, whereas others recommend screening to continue equally long every bit the adult female is in good overall health and has a life expectancy of more than years. To reach a conclusion, yous and I demand to discuss your overall health, review the risks and benefits of screening, and then make up one's mind together what the all-time selection would be for you lot.
2. Option Talk
You talk over individual comorbidities and potential risks and benefits of standing to do screening mammography.
Example: When nosotros accept into consideration your historic period, weight, lack of pregnant medical conditions, and the ease with which y'all are able to perform normal daily activities, we run into that mammograms may assistance you lot live longer. Studies bear witness that the potential do good of screening mammograms (ie, reducing breast cancer mortality) occurs ∼5 to 10 years afterwards mammography. Because you are likely to live longer than that, screening mammograms may benefit you. Was that clear? What questions do you have for me?
Case: When we look at your list of medical bug too as your age, the potential harms of screening mammography may outweigh the benefits for yous. Would you be willing to undergo surgery, and potentially other treatments if a mammogram were to diagnose a chest cancer? What questions do you take well-nigh whether to continue breast cancer screening?
Next, you lot use a patient decision assistance to review the potential harms and benefits of screening mammography in older women. You explain to your patient the risks of false positives and overdiagnosis, likewise as the potential mortality benefit, and show her the pictographs that convey this data in the decision assistance. Briefly, you review the treatment options for chest cancer, so that each patient considers whether or not she would cull treatment, if cancer was found on her mammograms. Afterward, you assess your patient's understanding.
Example: The benefit of screening mammograms is catching a cancer while it is modest, improving the run a risk that y'all will merely need minor surgery. Studies suggest that, amidst women who go screening mammograms, i less woman out of a one thousand will die of breast cancer in the next 5 years.
At that place are several potential harms of screening mammograms as well. For case, 100 women out of a thousand will experience fake positives in the next 5 years, equally y'all tin see in this graph. These false positives tin can cause pain, anxiety, and lead to additional tests. Overdiagnosis, which is finding a cancer that would non have harmed yous in your lifetime, is another harm of screening, and the adventure for overdiagnosis increases with age. If breast cancer is found, your treatment options are surgery, hormonal therapy, and radiation therapy. Each of these options has risks for side furnishings and complications, as briefly described in this determination assistance.
To make sure that I explained everything clearly, can you tell me in your ain words most the risks and benefits of screening?
three. Decision Talk
Now that you have discussed whether screening mammograms are likely to benefit Jane and reviewed the risks and benefits of screening with her, you ask your patient about her preferences for screening.
Example: At present that we've discussed screening in more than item, can you share your thoughts with me? Practise the harms of screening concern you more, or do you remember that the potential for finding a breast cancer early outweighs the risks of screening?
Last, y'all integrate your patient's preferences and values into the terminal decision and remind her that you tin can revisit this discussion in the futurity likewise.
Example: To summarize, you understand the risks of continuing with breast cancer screening, but you would still like to get biannual mammograms. You've had close friends that passed away from breast cancer, and standing with screening will give you some peace of mind. Is that correct?
I will order the mammogram for yous. Delight know that nosotros can always talk about screening again at your next appointment.
Concluding, framing discussions in terms of the balance between potential benefits of screening and harms has been found to be more effective than simply citing national guideline recommendations.43⇓ ⇓–46 This residuum is especially of import when explaining that screening mammograms would not be beneficial for a person with multiple comorbidities and a life expectancy of less than 10 years. In women with a shorter life expectancy, information technology is of import to emphasize that the patient is more likely to experience harms than benefits from breast cancer screening. Focusing on interventions that are likely to help the patient over a shorter time frame will likely provide more value. Additional strategies, videos, and exercise phrases for communicating prognosis to patients tin can be found on the ePrognosis website.47 Literature suggests that patients prefer to hear recommendations most screening cessation in the context of their other health conditions, rather than being told that they should stop screening.45,46
Conclusion
Although guidelines are conflicting about whether to proceed screening mammography in older women, clinicians tin can use shared determination making to aid women make decisions about screening. Using these communication strategies and decision aids along with life expectancy calculators, clinicians can fully appoint older women in the breast cancer screening process.
Notes
-
This article was externally peer reviewed.
-
Funding: There has been no extramural funding to support this work.
-
Conflict of involvement: None.
-
To come across this article online, delight become to: http://jabfm.org/content/33/three/473.full.
- Received for publication Oct 16, 2019.
- Revision received December 17, 2019.
- Accustomed for publication Dec 18, 2019.
References
- i.↵
- 2.↵
- 3.↵
- iv.↵
- five.↵
- half-dozen.↵
- 7.↵
- viii.↵
- 9.↵
- 10.↵
- xi.↵
- 12.↵
- xiii.↵
- fourteen.↵
- xv.↵
- 16.↵
- 17.
- 18.↵
- 19.↵
- 20.↵
- 21.↵
- 22.↵
- 23.↵
- 24.↵
- 25.↵
- 26.↵
- 27.↵
- 28.↵
- 29.↵
- 30.↵
National Comprehensive Cancer Network [Internet]. Chest cancer screening and diagnosis. Version 1. 2016. Available from: https://www.nccn.org/.
- 31.↵
- 32.↵
- 33.↵
- 34.↵
- 35.↵
- 36.↵
- 37.↵
- 38.↵
- 39.↵
- 40.↵
- 41.↵
- 42.↵
Schrager SL [Internet]. Breast cancer screening shared decision making toolkit. Madison: Academy of Wisconsin-Madison School of Medicine & Public Health; 2018. Available from: https://www.hipxchange.org/ScreeningMammo.
- 43.↵
- 44.↵
- 45.↵
- 46.↵
- 47.↵
- 48.
Practice bulletin number 179: breast cancer risk assessment and screening in average-gamble women. Obstet Gynecol 2017;130: 241–iii.
- 49.
- 50.
- 51.
- 52.
Royal Australian College of General Practitioners. Guidelines for preventive activities in general practice. 9th ed. East Melbourne: Royal Australian College of General Practitioners; 2018.
Source: https://www.jabfm.org/content/33/3/473
0 Response to "Breast Cancer in White American Women Peer Reviewed"
ارسال یک نظر